Why Endometriosis Is So Difficult to Diagnose, and How Imaging Can Help
March is Endometriosis Awareness Month, a time to talk about a condition that affects millions of women, yet often goes undiagnosed for years. It affects approximately 1 in 10 women of reproductive age, and many women end up waiting years for answers. If you or a loved one has struggled with chronic pelvic pain, painful periods, or unexplained fertility challenges, you may already understand one of the biggest issues surrounding endometriosis. It can be very hard to diagnose.
What is Endometriosis?
Endometriosis occurs when tissue similar to the lining of the uterus grows outside of it, involving the ovaries, fallopian tubes, pelvic ligaments, or other surrounding structures. Unlike normal uterine lining, this tissue has no way to exit the body during a menstrual cycle. Symptoms can vary widely, from severe pain during intercourse to fibroids or pelvic pain, heavy periods, gastrointestinal discomfort, or fertility challenges. Furthermore, symptoms don’t always match the severity of the disease; that variability is part of what makes diagnosis so complex. Many conditions can overlap in presentation, and historically, the only way to definitively diagnose endometriosis was through surgery. But not anymore.
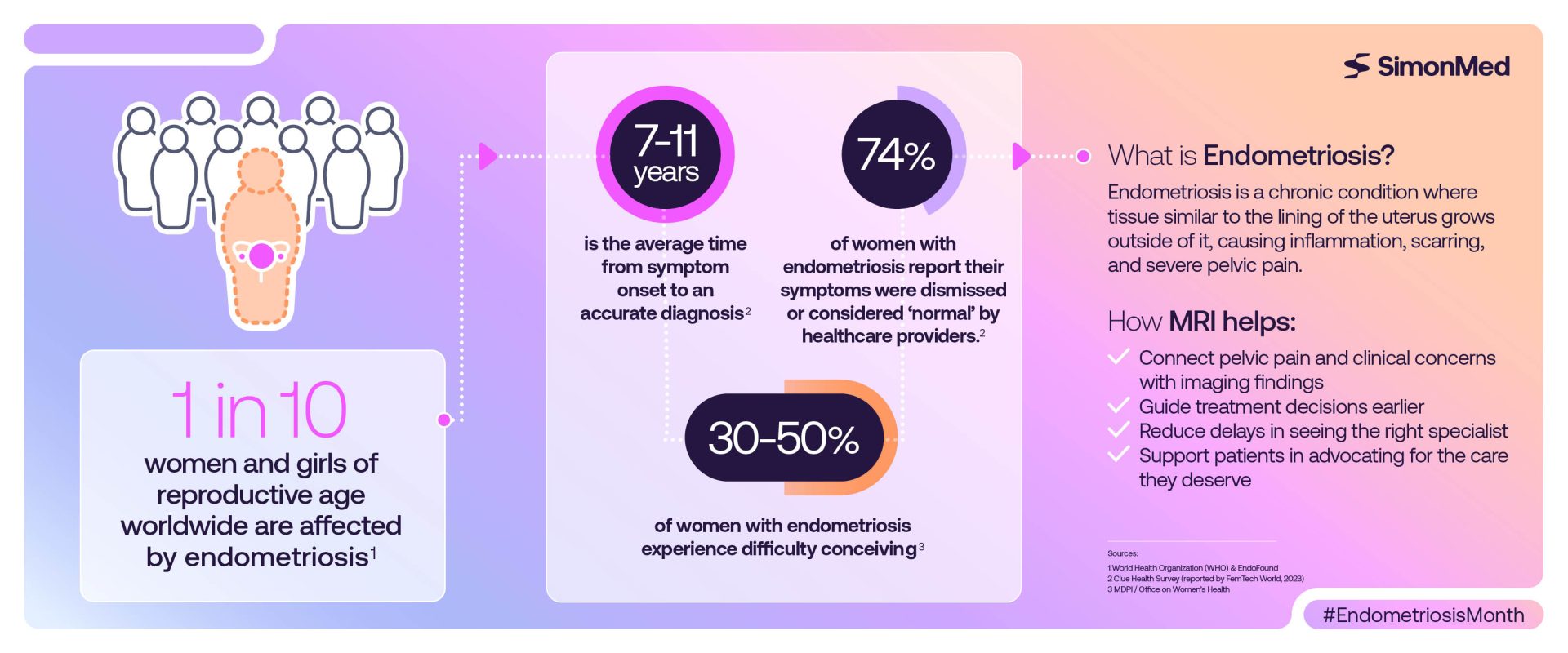
Why is Endometriosis often missed?
On average, women can wait years between the onset of symptoms and a confirmed diagnosis. There are several reasons:
1. Symptoms are often dismissed
Painful periods are frequently normalized. Many patients are told their symptoms are “just part of being a woman,” which can delay further evaluation.
2. Symptoms overlap with other conditions
Endometriosis can mimic irritable bowel syndrome (IBS), pelvic inflammatory disease (PID), ovarian cysts, or other gynecologic disorders.
3. It doesn’t always show clearly on imaging
Historically, the only definitive way to diagnose endometriosis has been through laparoscopic surgery. While imaging can strongly suggest the presence of disease, some forms of endometriosis may not be visible on imaging, which can make diagnosis more challenging.
“Endometriosis isn’t a one-size-fits-all condition,” Dr. Simon explains. “It can look different from patient to patient, which means diagnosis requires careful clinical and imaging evaluation.”
The role of pelvic MRI
Pelvic MRI (Magnetic Resonance Imaging) provides highly detailed images of soft tissues and can identify many forms of moderate to severe endometriosis. It plays an important role in evaluating suspected cases.
When symptoms strongly suggest endometriosis, an MRI can:
- Help correlate symptoms with imaging findings
- Guide treatment decisions earlier
- Reduce delays in referral to the right specialist
- Support surgical planning when needed
Pelvic MRI clearly shows areas where endometriosis often hides, including:
- Ovarian endometriomas (cysts caused by endometriosis)
- Deep infiltrating endometriosis behind the uterus
- Possible involvement of the bowel, bladder, or pelvic ligaments
MRI’s superior soft tissue contrast allows radiologists to assess the extent of disease more precisely, especially when ultrasound findings are limited or inconclusive.
In many cases, MRI findings provide highly actionable information that can help guide next steps in care.
“A well-performed pelvic MRI can give clinicians a roadmap,” says Dr. John Simon, Founder and CEO of SimonMed. “It helps guide next steps with clarity and confidence.”
When MRI findings are present, they can significantly shorten the path to diagnosis and treatment planning.
Transparency about these limitations is essential, and it’s worth remembering that imaging is only part of the diagnostic process.
Safe and noninvasive
Pelvic MRI uses no radiation. In many cases of suspected endometriosis, specialized non-contrast MRI sequences are sufficient. Contrast may be used selectively to clarify complex findings.
For women experiencing persistent pelvic pain, MRI offers a noninvasive way to gain more information, without immediately turning to surgery. Imaging is only one piece of the larger diagnostic puzzle, which also includes physical exam findings and physician expertise.
Why earlier answers matter
Delayed diagnosis can take a physical and emotional toll when chronic pain affects daily activities, relationships, work performance, and mental health.
Earlier imaging can:
- Validate patient concerns
- Strengthen communication between patient and provider
- Help guide appropriate referrals
- Support more personalized treatment planning
Earlier and more accurate detection can help patients and their physicians make informed decisions about medical management, fertility planning, or surgical options.
Most importantly, it reinforces a simple but powerful truth: your symptoms are real.
“When patients have better information, they can make decisions with confidence, instead of continuing to live in uncertainty,” says Dr. Raj.
If you’ve been told your pain is normal but it doesn’t feel normal, that matters. Persistent pelvic pain deserves evaluation. Severe menstrual symptoms deserve attention.
Diagnosis starts with being heard.
Looking ahead
Advances in imaging and artificial intelligence continue to improve how we evaluate complex conditions like endometriosis. Emerging AI-enhanced MRI tools hold promise for further improving detection and consistency in interpretation.
As these technologies evolve, the goal at SimonMed remains the same: to help more women receive clearer answers sooner. No one should have to wait years to understand their pain, because your symptoms deserve answers.
Resources: Office on Women’s Health, Cleveland Clinic, World Health Organization